
PICTURED:
IndyCar Series driver Charlie Kimball is featured in an innovative research project in collaboration with Assistant Professor David Ferguson. Photo courtesy of LAT Photo USA.
Kinesiology scholar pioneers research to fuel athletic excellence—and drive change for diabetes in sports
By Lauren Ebelt
Upon first glance, it doesn’t look like much.
It’s a clear plastic box atop a metal gurney, accompanied by some wooden blocks, cushions and a bicycle seat. Small machines with wires draping down sit on top, blinking and ready to collect data. Next to the whole contraption is a large, cylindrical vacuum connected by a hose.
The machine, aptly called The Box, looks like something you could make out of spare parts in a garage. And in a way, it was. It was built 30 years ago using odds and ends and whatever worked. But the original theory behind it helped prove that we could send humans to the moon.
Today, The Box is making history again.
In his laboratory space in IM Circle at Michigan State University, Assistant Professor of Kinesiology David Ferguson is using it to help change the way we see athletes, motor sports and diabetes.
Astronauts and athletes
Racing and cars have always been in Ferguson’s life.
When he was younger, he often tinkered with vehicles, “fascinated” by them, and by racing itself. While attending the University of Nevada, Las Vegas, pursuing a bachelor’s in kinesiology, he even raced in the Sports Car Club of America.
Academia, however, took him down a different road. Ferguson shifted his focus to health, studying how early life nutrition influences cardiovascular function later in life, which he continues to research today. He earned a master’s from the University of North Carolina, Charlotte and a Ph.D. from Texas A&M University, both in exercise physiology. He also gained postdoctoral experience in pediatrics and molecular physiology at Baylor College of Medicine.
Ferguson was first introduced to The Box by J. Timothy Lightfoot, his mentor at UNC Charlotte as well as Texas A&M, where Lightfoot is now a professor of health and kinesiology with a joint appointment in genetics.
In the 1980s, while Lightfoot was working on a fellowship at the National Aeronautics and Space Administration (NASA), he helped to test how astronauts reacted being sent to and coming back from space.
He took the same theory and methodologies of the test with him to Johns Hopkins University, and in 1986, created The Box. It tested the maximal gravitational forces (G-forces) a person could tolerate by subjecting the lower body to negative pressures. It was a newer model than what had been used at NASA, and with added improvements. For the first time, The Box was made to withstand higher pressures, and actually expose an individual to conditions physiologically simulating higher G-forces.
The Box traveled with Lightfoot across his career. But since the late-1990s, when he last used The Box in research, it had more or less been collecting dust.
That is until David Ferguson had an idea—combining his research on exercise physiology and his passion for racing.

Assistant Professor David Ferguson (left) and IndyCar driver Charlie Kimball have collaborated since 2011 to improve Kimball’s athletic performance. Photo courtesy of Derrick L. Turner / Communications and Brand Strategy.
“I think you suck on oval tracks—and I think I know why”
Ferguson has always found ways to incorporate racing in his career. While at UNC Charlotte, he was conducting research with NASCAR, studying pit crews’ core body temperatures and how that related to their pit stop times (see “Every Second Counts,” below).
Coincidentally, Ferguson happened to watch the 2011 Indianapolis 500, a 200-lap, 500-mile race held annually on Memorial Day weekend. It was then that he first heard about racer Charlie Kimball. Kimball, who has Type 1 diabetes, made history when he became the first professional driver with diabetes to finish the Indy 500.
“My first thought was ‘this is going to be really good data. I wonder if I can get my hands on that data. I wonder what his blood glucose is doing during the race,’” Ferguson remembered.
Through Kimball’s website, Ferguson proposed an in-person meeting where Kimball would undergo rigorous physical assessments that could help pinpoint his strengths and weaknesses. His stance was simple: “I think you suck on oval tracks—and I think I know why.”
It was true: Kimball admitted the curvy, oval tracks weren’t his forte. He knew he was making too many mistakes on ovals, but didn’t quite know what to do about it.
With the data Ferguson was suggesting, they could determine how to help Kimball reach his peak performance.
Ferguson’s idea was enough to get Kimball interested, and in 2011—the same year Kimball made history at the Indy 500—the two met at Texas A&M. Their collaboration has continued ever since.
In addition to training and rehabilitation (and Ferguson working closely with Kimball’s endocrinologist), Kimball has endured a variety of annual tests:
- BodPod test: evaluating the percentage of body fat and muscle mass
- Wingate bike test: measuring skeletal muscle power output
- VO2 max test: determining aerobic capacity and fitness level utilizing a treadmill
- Lower body negative pressure chamber test (The Box): measuring G-force tolerance
The Box came to MSU along with Ferguson in 2015, and is one of the few of its kind outside of NASA or the military able to test G-force tolerance.
Each test, administered in the Human Energy Research Lab at IM Circle, tells Ferguson and his graduate assistants intricate details about what is going on in Kimball’s body—and what he can endure.
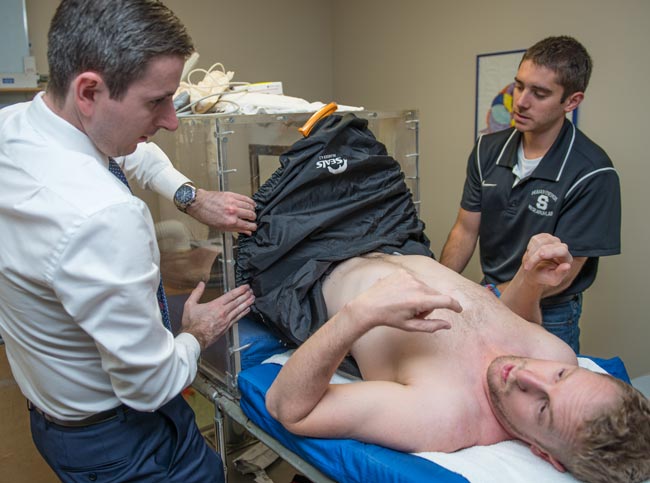
Ferguson (left) and research assistant Todd Buckingham seal Kimball into The Box. Photo courtesy of Derrick L. Turner / Communications and Brand Strategy.
Under (negative) pressure
Driving a race car isn’t as easy as it may appear.
With each turn on a track, drivers experience a substantial amount of G-forces, requiring them to have intense physical stamina. In fact, on high-banked oval courses, drivers are on such a steep incline that they are often sitting sideways as they zoom around the curve. As drivers experience high G-forces, blood begins to pool in their legs.
Thus, it is essential that drivers not only react quickly, but also have the aerobic and strength capacity to counteract these G-forces.
“The problem with blood pooling and G-forces in the car is that any reduction in oxygenated blood to the brain reduces my ability to think clearly and make split-second decisions,” Kimball said. “One of the things we’ve learned is there is a correlation between poor blood sugar management and G-resistance.”
That’s why Kimball and Ferguson turned to The Box.
An individual’s G-force tolerance is influenced by a variety of things, including height and cardiovascular fitness; the pressure chamber is able to give them an idea of how many G-forces Kimball can take.
During the test, Kimball is sealed into The Box so no air can get in. He is attached to blood pressure machines, heart monitors and an electrocardiogram (EKG). Then, with a low whir, The Box is brought to life.
The test begins with gathering baselines of measurements, but even early on, Kimball is able to feel a difference. The pressure feels as if he is being “pulled down into” the box, and he can feel his legs getting warmer as the blood begins to pool, simulating what happens to Kimball in the car.
For however long he can endure it, a vacuum continues to suck pressure out of The Box.
Before long, Kimball’s legs become pink and puffy, veins pop out and he begins sweating. His language becomes more slurred and at times he repeats himself. This is another example of the blood being pulled away from the brain, Ferguson says.
In a word, it is “uncomfortable,” says Kimball.
When health and safety issues arrive—cardiac arrhythmia, a sudden drop in heart rate or blood pressure, to name a few—or if Kimball feels the test is becoming too much to handle, the test can be stopped at any time.
Stopping brings great relief: Instantly the stress is lifted from Kimball’s legs after 30 minutes of being exposed to increasing G-forces. At the maximum pressure in a recent test, he was experiencing the same physiological response as 7.5 Gs.
The force is substantial. At 7.5 Gs, Kimball was experiencing 7.5 times the average pull of gravity. For example, if his head weighs 11 pounds regularly, it weighs 82.5 pounds in that moment. The pressure he was able to withstand, even for a short period of time, was greater than what he typically experiences during races, where he is usually combatting 4 to 5 Gs per turn.
Over the course of six years in the study, Kimball has developed a G-force tolerance that is considered high for the average population.
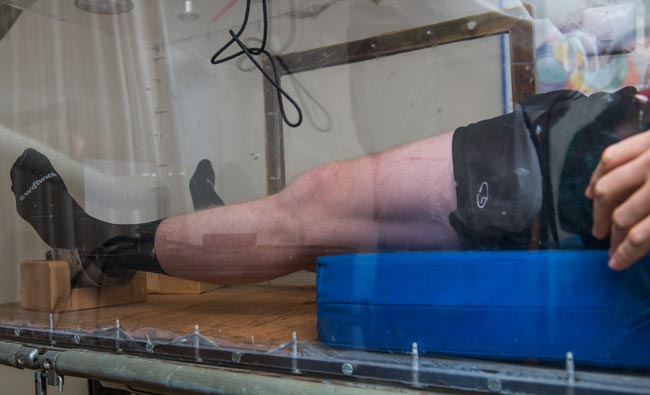
Inside The Box, Kimball is exposed to increasing gravitational forces (G-forces) to simulate what he experiences in his IndyCar. Photo courtesy of Derrick L. Turner / Communications and Brand Strategy.
Science and gambling
The Box did more than expose Kimball to G-forces. It also answered an integral question to his racing success: What is his ideal blood glucose level?
Blood glucose (blood sugar) levels vary throughout the day. It can depend on when and what was last eaten, age, weight and other factors. What is considered normal for one individual could be different for others, especially for those with diabetes. Ferguson’s challenge was to find what worked best for Kimball, for his health and his performance.
“I spent some time trying to read about optimal blood glucose for performance, and it’s not there,” Ferguson said. “There are a lot of athletes with diabetes, so this was surprising.”
With a lot of science, and some guesswork, they were able to pinpoint an answer for Kimball.
Kimball’s assistant engineer charted blood glucose levels during the race, position in the race, time behind the leader and a general competitive lap time for three years. That data was sent to Ferguson to analyze the performances, and see if there was any correlation.
“Can we figure what blood glucose number he is doing well at?” Ferguson asked. “We can take lap time, finishing position … but you also have to account for competition. How do you assess competitive skill? We used the odds generated by Las Vegas on if the drivers would win the championship. It’s a little bit of science, and a little bit of gambling.”
All of the data from his physical assessments and races were pulled together. Using a regression analysis, Ferguson was able to predict success—and to find a number.
He determined that Kimball operates best with a blood glucose number of 147 mg/dl-1, or milligrams per deciliter.
“With low blood sugar, Kimball’s reaction time was slower than what was ideal for competition,” Ferguson explained. This is a detriment to performance, where every millisecond counts in the high-speed world of IndyCar. “At 120-170 mg/dl-1, his reaction is really quick. Any higher than that, he still has a fast reaction time, but it’s not the optimal point we’re looking for.”
To get to that magic number, Kimball is extremely diligent about blood sugar management and testing. He makes sure to eat properly before the race. And during the race, he has the option of drinking orange juice to maintain the appropriate levels if needed (see “Inside Kimball’s IndyCar,” below).
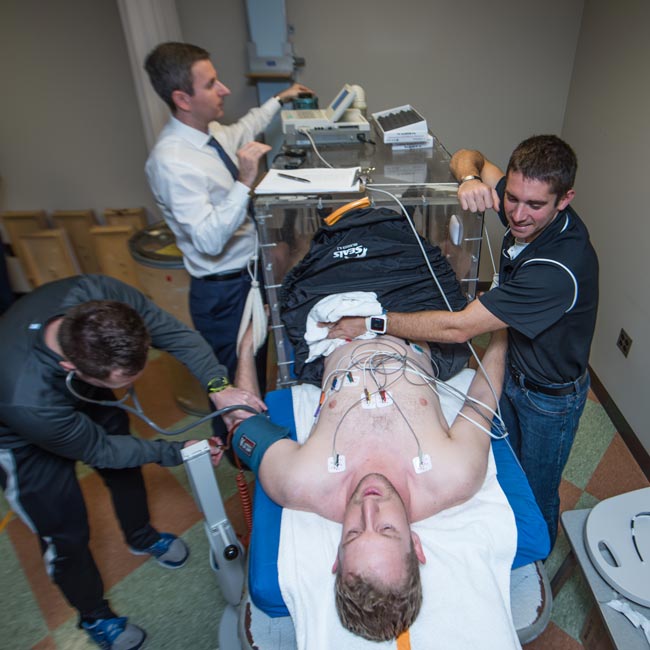
Ferguson and his team monitor Kimball’s vitals during the testing. Photo courtesy of Derrick L. Turner / Communications and Brand Strategy.
Successful track record
The years of rigorous testing are paying off.
“Working with Ferguson has allowed me to do what I do even better,” Kimball said. “The data and information is continuing to improve my results and performance. Having worked with Ferguson, my training has evolved. Rather than just endurance and cardiovascular work, I work toward balancing that with strength and power. Being able to look at this information and see how my body works not only makes my training better, but allows me to better measure my diabetes.”
Of the 2,070 race laps in the 2016 season, Kimball was able to complete 2,066 (99.8 percent)—more than any of his competitors throughout the season—and he finished in the top-10 in championship points. He has also been in the top-5 in the Indy 500 in the past two seasons.
“Everything we do is data-driven, and that’s why we’ve been successful,” Ferguson has said about the extensive research project.
Ferguson’s research is notable across racing: He also works with other drivers in the IndyCar Series, Formula 1, NASCAR and the International Motor Sports Association (IMSA). In fact, he recently received a grant from Hintsa Performance to “look at the mental and physical requirements to develop a kid to become a Formula 1 driver.” Hintsa Performance, based in Europe, utilizes a holistic approach—including modifications to physical activity, nutrition and sleep—to improve the well-being of athletes, entrepreneurs and more.
Ferguson’s research is rare in a field that, for the most part, is largely uncovered. Since 1964, there have been less than 30 articles published on motor sports.
Ferguson’s latest contribution to the research—the first of its kind to evaluate physiological stress on a driver over multiple years—helps an increasing number of diabetic race car drivers. Since Kimball began racing, at least one has joined him in competing in the IndyCar Series, and another competes full-time for NASCAR. According to Ferguson, it is estimated that anywhere from 25 to 125 people with Type 1 diabetes are racing in various leagues across the United States.
And the impact does not end with racing alone; athletes with diabetes, including on the amateur, professional and Olympic levels, compete in sports around the world.
“This research will help any athlete with diabetes,” Ferguson added. “Diabetes is no longer a sentence to be inactive.”
Watch this video from MSU Today to learn more about how Ferguson’s research is helping Kimball “outpace diabetes:”
Every second counts
In 2010, while working with NASCAR, Ferguson tested pit crews’ core body temperatures across several races. The results were definitive: They were hot.
Ferguson and his research group hypothesized that if pit crews practiced during the heat of the day, when their bodies would learn to acclimate to the heat, their pit crew times would be shorter.
In a championship race, Tony Stewart’s pit crew members, who had followed the suggestions of Ferguson, were 1.5 seconds faster at each stop than their competitors—and eventually went on to win.

Photo courtesy of LAT Photo USA.
Inside Kimball’s IndyCar
“My car is different from everyone else because I am different,” said Kimball.
To keep him—and his competitors—safe during races, he must monitor his glucose levels. Both his car and body data are displayed on the wheel of his car, and he wears a dermal continuous glucose monitor that wirelessly transmits data during the race.
If his glucose levels fall, he has a tube running from his seatbelt to his helmet with orange juice to replenish his system. He also has a supply of water on his seatbelt for further hydration.
The basics of diabetes
Kimball was diagnosed with Type 1 diabetes when he was 22 years old. According to the American Diabetes Association (ADA), only 5 percent of those with diabetes have this form of the disease, where the body does not produce insulin.
“The body breaks down the sugars and starches you eat into a simple sugar called glucose, which it uses for energy. Insulin is a hormone that the body needs to get glucose from the bloodstream into the cells of the body,” the ADA explains.1
Another form of diabetes, Type 2, is the most common form, in which the body has higher than normal blood glucose levels.2
1. American Diabetes Association: diabetes.org/diabetes-basics/type-1




